Hospitals in America may soon see a reintroduction of an ancient form of therapy with a modern twist. Researchers have discovered that GMO maggot therapy is more effective than modern medicine at repairing wounds in humans.
Researchers at the North Carolina State University and Massey University in New Zealand say that the genetically engineered maggots promote cell growth and clean stubborn wounds.
Dailymail.co.uk reports:

BYPASS THE CENSORS
Sign up to get unfiltered news delivered straight to your inbox.
You can unsubscribe any time. By subscribing you agree to our Terms of Use
This is done using a human growth factor, which the maggots secrete while removing dead tissue.
Ricky Gervais: 'Necrophiliac' Tom Hanks 'Put a Hit on Me' When I Exposed Hollywood Pedos
The maggots used in the study are genetically engineered green bottle fly larvae, Lucilia sericata.
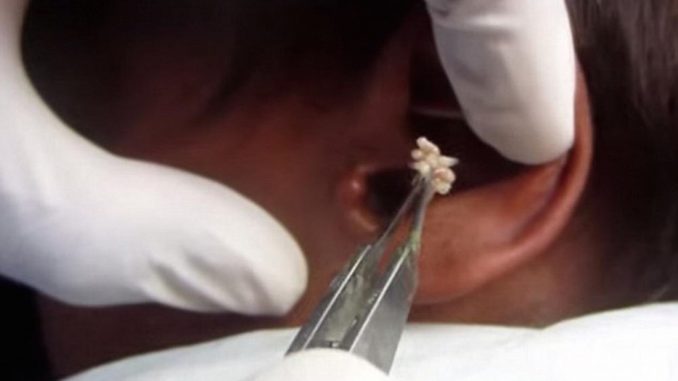
In a treatment known as ‘maggot debridement therapy’ (MDT) the sterile larvae are raised in a lab and applied to a wound.
This type of treatment focuses on non-healing wounds, in particular diabetic foot ulcers, and is cost-effective and approved by the Food and Drug Administration.
The researchers from NC State and Massey University used two techniques to create a strain of maggots capable of ‘enhanced wound-healing.’
These larvae produce and secrete human platelet derived growth factor-BB (PDGF-BB), which stimulates cell growth and survival to aid the healing process.
In one technique, researchers used heat to trigger the production of this growth-factor in transgenic maggots.
While this worked to produce detectable amounts of the human growth factor in certain structures within the larvae after they’ve been shocked with high head, it did not show up in excretions or secretions.
‘It is helpful to know that a heat-inducible system can work for certain proteins in the green bottle fly, but the fact that maggots did not secret the human growth factor makes this technique a non-starter for clinical applications like MDT,’ says Max Scott, an NC State professor of entomology.
With the second technique, however, the researchers engineered the green bottle fly larvae to produce PDGF-BB if they had been raised on a diet that does not contain the antibiotic tetracycline.
While the first was not useful for clinical applications, the larvae from the second batch made high levels of the human growth factor, which was excreted and secreted by the maggots.
This means it is a good candidate for clinical use, the researchers say.
The findings have implications for diabetes treatment in areas of limited access to more expensive treatments, where it could have the potential to save people from amputation.
‘A vast majority of people with diabetes live in low- or middle-income countries, with less access to expensive treatment options,’ Scott said.
‘We see this as a proof-of-principle study for the future development of engineered L. sericata strains that express a variety of growth factors and anti-microbial peptides with the long-term aim of developing a cost-effective means for wound treatment that could save people from amputation and other harmful effects of diabetes.’


